Fenbendazole is a versatile medication frequently prescribed to treat parasitic infections in both animals and humans. It’s categorized under the benzimidazole group of drugs. Its primary function is to disrupt the energy-producing processes of the parasites, causing them to perish.
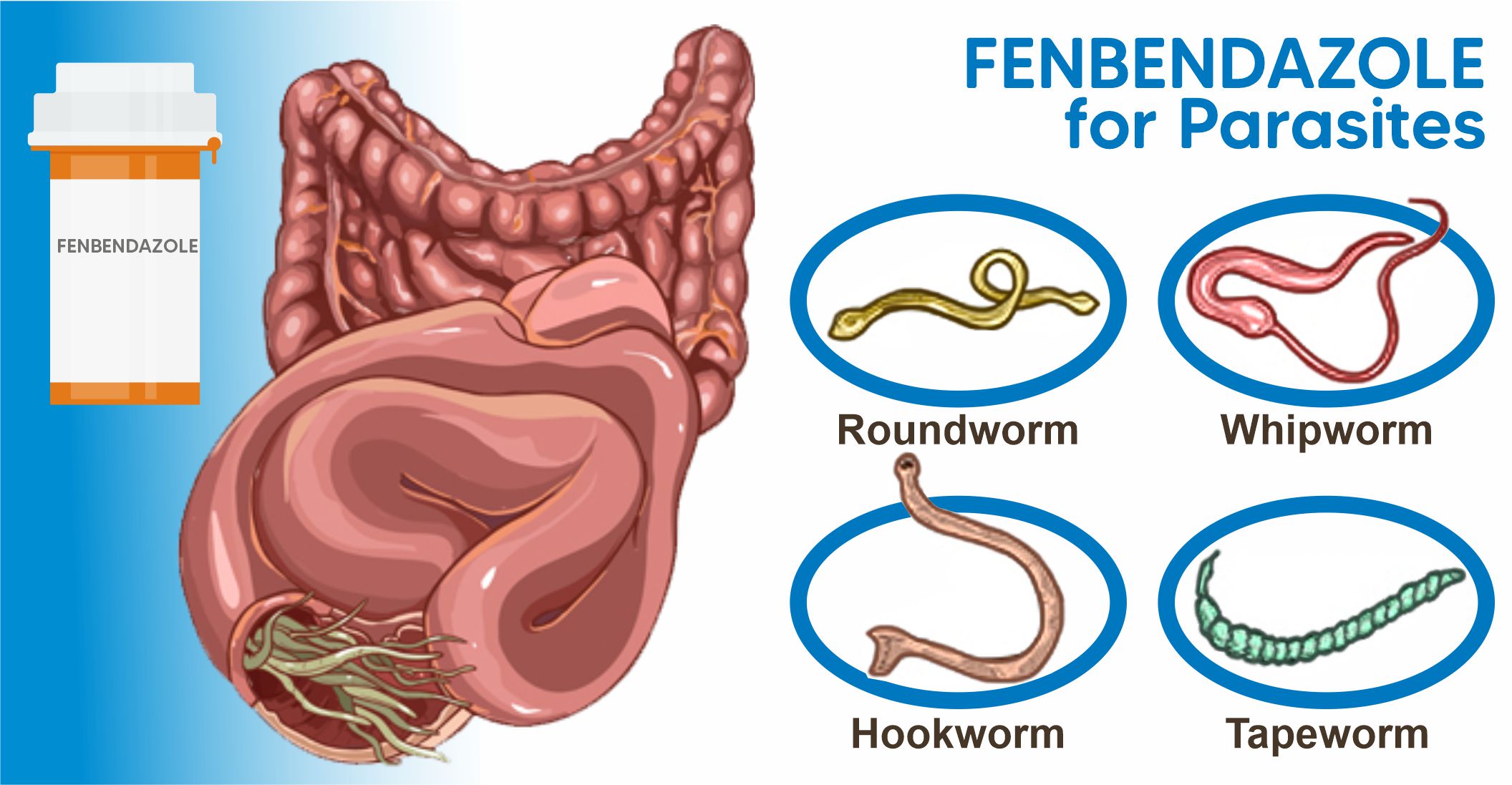
Globally, parasitic infections pose a considerable health challenge, impacting countless people and animals. Common culprits behind these infections include roundworms, hookworms, whipworms, and tapeworms.
Parasitic infections might not always show signs immediately, but over time, they can lead to various puzzling and challenging health issues:
- Nutrient shortages in diet,
- Cravings for sweets and certain foods,
- Swelling and discomfort in the stomach,
- A drop in red blood cells causing anemia,
- Constant tiredness,
- Elevated body temperature,
- Sweating during the night,
- Aching muscles and joints,
- Skin changes, like a reddish facial blush called rosacea,
- Itchiness near the rear end,
- Itching in the vaginal area.
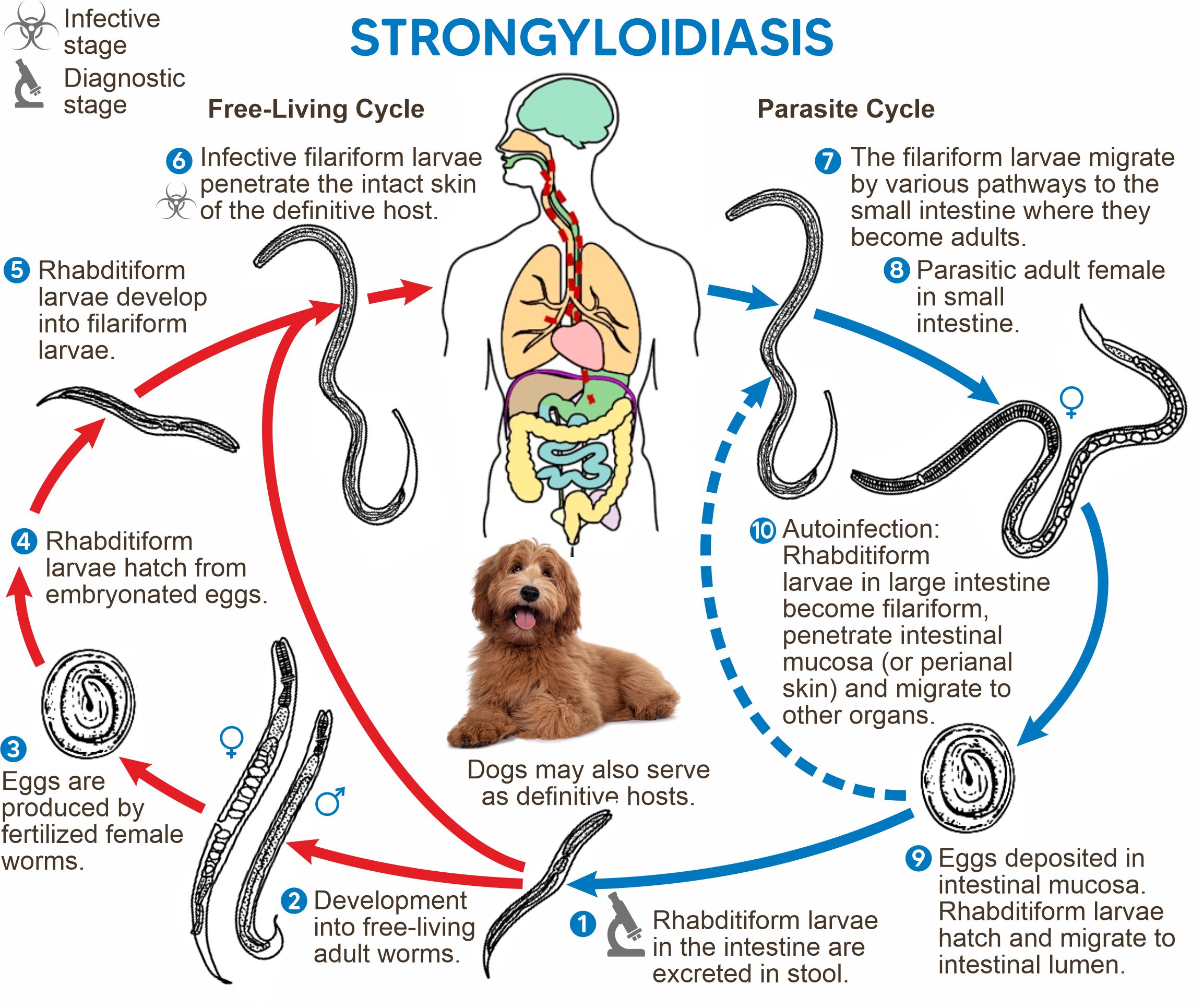
Fenbendazole has established its reputation as an effective treatment for gastrointestinal parasites. Its broad-spectrum action against various parasites makes it a cornerstone in managing these infections. Frequently, fenbendazole is recommended for the treatment of various worm-related illnesses, including strongyloidiasis, trichuriasis, and enterobiasis.
Fenbendazole for Parasites – How it Does Work?
Fenbendazole operates differently from other worm-fighting drugs. Its unique way of working targets a particular protein, called beta-tubulin, found in the tiny tube-like structures of parasites. Structures known as microtubules play a big role in many cell activities, including cellular division and reproduction.
When a parasite takes in fenbendazole, the drug attaches to the beta-tubulin inside these microtubules. The formation of microtubules is disrupted by this interference. This throws off the parasite’s ability to make more of its kind because it can’t reproduce its cells as it should.
Moreover, this drug messes with the parasite’s way of using glucose, which is like its fuel. By blocking how it uses this fuel, fenbendazole forces the parasite to run out of energy. Without energy, the parasite starves and dies.
The beauty of fenbendazole for human parasites lies in its precision. It specifically targets the beta-tubulin found within parasites, rather than affecting the same component in the host. So, while it’s doing its job on the parasites, it doesn’t harm the host animal’s cells. That’s why fenbendazole is seen as a safe way to get rid of parasites in many cases.
Fenbendazole’s Effectiveness in Treating Two of the Toughest Parasite Diseases
The Dangers of Roundworms (Ascarids)
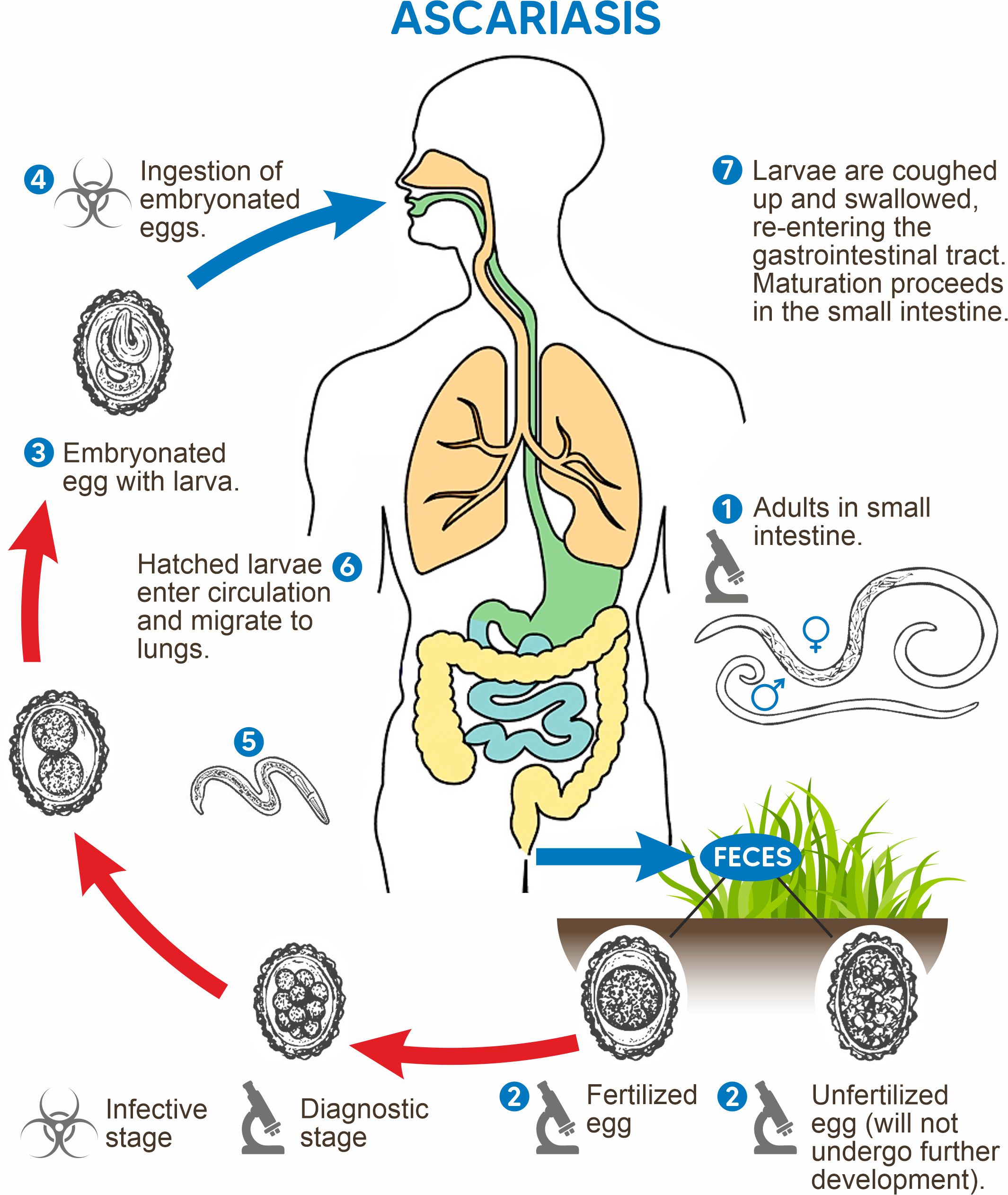
The presence of ascarids, commonly referred to as roundworms, has the potential to cause significant harm. Their life cycle goes like this: when their eggs are ingested, they reach our gut, where the worm larvae emerge. As they feed and grow, the larvae develop into adult worms in our digestive tracts and begin their journey.
In the lungs, these larvae are coughed out and swallowed, finally settling in the intestines where they grow into full-sized adults. And these adults aren’t tiny — they can be as long as 40 centimeters. In high numbers, they can block the intestines, potentially causing serious complications like impaction or even a tear, which could be deadly. However, there is something that we can do, no doubt.
Here’s where fenbendazole appears, a medicine that’s quite handy in such a situation. Fenben interrupts the ongoing cycle by specifically targeting the mature roundworms residing in the intestines, essentially starving these worms to death.
This approach is gentle but effective, reducing potential side effects that might happen when treating a heavy roundworm load using other medications.
Fenbendazole for human parasites is a prime option for killing roundworms due to its remarkable combination of delicacy and efficacy in action. Furthermore, it retains its effectiveness long after you start using it. In contrast, roundworms are becoming more resistant to other drugs like ivermectin, moxidectin, and pyrantel pamoate global
Encysted small strongyles
Small strongyles are a notable concern due to their sneaky behavior of encysting or “hiding.” Here’s how they do this: when a host ingests small strongyle larvae, these larvae travel through the stomach and get into the lower intestines. There, they dig into the intestine wall.
The tricky part? These larvae can then go dormant or “hide” by encysting within the wall. A staggering 90% can choose to encyst, staying in this halted state for anywhere from 4 months to a lengthy 3 years. With time, these hidden larvae pile up. When they decide to wake up all at once (often in spring), it can lead to major health issues for the host, and in worst cases, death.
This is where fenbendazole comes into play. Taking it for a longer period of time in the appropriate amount is the only known treatment that’s been shown to tackle every stage of these hidden strongyles.
What makes fenbendazole stand out? It has the unique ability to pierce through the protective layer of the intestines and eliminate these lurking larvae before they become a bigger problem.
Fenbendazole stays in the body for a good amount of time. It doesn’t break down so quickly. This prolonged presence ensures that it works well against dormant threats like the encysted small strongyles.
Strongyloidiasis can also be treated with ivermectin and albendazole, both of which are widely available.
Understanding the Basics of Parasite Management
Humans can be hosts to numerous parasites, ranging from those that can be seen with the naked eye to those that are tiny. It is quite remarkable that even in highly developed nations, there appears to be a considerable number of individuals who carry at least one type of parasite.
Parasites are incredibly widespread, making it considerably difficult to fully rid ourselves of their presence. And it’s not just about maintaining personal hygiene. Yes, certain parasites come from raw or undercooked food, but many others are simply present in our surroundings.
All parasites have one thing in common – they go through life cycles that involve producing egg sacs. Once a human is infected, the female parasite can lay a staggering 20,000 to 200,000 eggs daily.
Inside various locations within our bodies, one can come across these eggs safeguarded by protective sacs. Interestingly, as long as the mother parasite is alive, she releases chemicals that prevent these eggs from hatching. However, if she dies, these eggs hatch and potentially lead to another round of infection in places like the gut or liver.
In order to successfully eradicate parasites, it is necessary to tackle both the fully grown organisms and their egg sacs simultaneously. Many chronic inflammatory illnesses that we can’t cure could, in theory, be the result of the body’s continual (and often futile) attempt to eradicate these egg sacs. If left unchecked, the number of these sacs will only grow, leading to increasing inflammation as the body continues its attempts to expel these unwelcome guests.
In order to effectively combat parasitic infections, it is of utmost importance to embrace a treatment strategy that follows a cyclical pattern. Simply using the fenbendazole improperly might not target the egg sacs, leading to ongoing inflammation in the body.
Starting a treatment for parasites may lead to noticeable symptoms, including changes in bowel movements, the presence of gas, or even diarrhea. It’s essential to maintain consistency in treatment by ensuring there’s no more than a 2-3 week gap between sessions. This duration is known as the “cycle length.” Extending this cycle might provide a window for a more significant number of parasite eggs to hatch and mature. When you eventually administer the next round of treatment, you might end up killing a vast number of parasites at once. This could trigger a significant allergic response, known as the Herxheimer reaction (named after the doctor who first detailed the phenomenon). Symptoms of this reaction can start with minor histamine-induced issues like sneezing or watery eyes but can escalate to more severe symptoms like fever, rapid heartbeat, shortness of breath, brain fog, and even emotional instability. Using shorter treatment cycles can generally help avoid this reaction.
If an individual doesn’t show signs of inflammation or other health issues linked to parasites, it’s advised for adults to undergo treatment for about two months. It’s beneficial to alternate between medications with slightly different mechanisms of action. I’ve provided a detailed list of treatment options below, but I’ll also share my personal regimen and its ongoing results. Subsequently, a monthly maintenance treatment might be appropriate. For younger children, a reduced treatment duration and dosage are recommended. Consulting a skilled pediatrician for guidance is always a wise move.
How Intestinal Parasites Enter Our System
Intestinal parasites can find their way into our bodies through various means. Here are the primary ways one might acquire these unwanted guests:
- Consuming undercooked or raw meat from an infected source, such as cows, pigs, or fish.
- Drinking water that has been contaminated with parasites.
- Ingesting soil tainted with parasitic organisms.
- Direct contact with infected feces.
- Living in or traveling to areas with inadequate sanitation facilities.
- Neglecting proper hygiene practices, like not washing hands regularly.
- Age plays a role; both children and the elderly are more susceptible to infections.
- Frequenting child care or institutional care centers can increase exposure risk.
- Possessing a compromised immune system makes one more vulnerable.
- Those with conditions like HIV or AIDS are at a heightened risk.
Upon ingesting or coming into contact with these contaminants, the parasites navigate to the intestines. Here, they multiply and flourish. As their numbers grow and they increase in size, the infected individual may start to notice symptoms.
Types of Intestinal Parasites
Tapeworms
Tapeworms are intestinal parasites that humans can contract, mainly from consuming undercooked pork or beef. The main species that can infect humans are:
- Taenia saginata: Commonly referred to as the beef tapeworm.
- Taenia solium: Known as the pork tapeworm.
- Taenia asiatica: Often termed the Asian tapeworm.
In the United States, it is believed that fewer than 1,000 individuals contract tapeworms annually. However, the precise number remains uncertain.
Pinworm
A pinworm infection is the most prevalent intestinal worm infection in the United States and ranks among the top worldwide. It’s especially common among school-going children. The minuscule pinworm eggs are easily passed from one child to another, making this group particularly vulnerable.
Symptoms:
People with pinworm infections might experience:
- Itchiness around the anal or vaginal regions.
- Sleep disturbances, moodiness, grinding of teeth, and general restlessness.
- Stomach discomfort and occasional nausea.
How It Spreads:
The root cause of a pinworm infection is unintentionally consuming or inhaling pinworm eggs. These tiny eggs, which are microscopic in size, can be transferred to your mouth through contaminated edibles, beverages, or even by touching them and then touching your mouth. After being ingested, these eggs travel to the intestines where they evolve into adult worms in just a matter of weeks.
Hookworms
Hookworms are parasitic nematodes that live in the intestines of their hosts, which include humans. They are known to cause various symptoms and are typically acquired through direct contact with contaminated soil.
Symptoms:
People infected with hookworms might exhibit:
- A rash on the feet, often a telltale sign indicating the point of entry of the larvae.
- Febrile conditions.
- Respiratory symptoms such as coughing or wheezing.
- Gastrointestinal discomfort including abdominal pain, decreased appetite, and diarrhea.
- Noticeable weight reduction.
- Signs of anemia, resulting from the blood-sucking activity of the adult worms.
Transmission:
The life cycle of hookworms begins with the laying of eggs in the intestines, which are then expelled through feces. When infected individuals defecate outdoors or if human feces are used as a fertilizer, the soil becomes a reservoir for these larvae. Direct skin contact, particularly when walking barefoot on contaminated soil, can lead to infection as the larvae penetrate the skin.
Potential Complications:
The primary concern with hookworm infections is the blood loss they cause, as these worms thrive by feeding on blood. Persistent, untreated infections can cause:
- Anemia: This is marked by symptoms like fatigue, dizziness, shortness of breath, chest pain, and muscle cramps.
- Protein Deficiency: This is particularly concerning in children, causing stunted physical and cognitive growth.
Treatment:
Hookworm infections can be diagnosed through stool examinations and blood tests. Once diagnosed, they are treated with anthelmintic medications. These drugs are designed to eliminate the worms from the intestines.
Commonly prescribed medications for hookworms include:
- Mebendazole: An oral drug that targets a wide range of intestinal worms.
- Albendazole: Another broad-spectrum antiparasitic drug.
- Fenbendazole: Primarily used in veterinary medicine, but can also be effective against some human parasitic infections.
After treatment, it’s essential to maintain good hygiene and avoid walking barefoot in potentially contaminated areas to prevent reinfection.
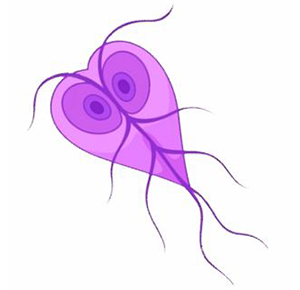
Giardia
Giardia is a protozoan parasite that causes an intestinal infection known as giardiasis. The illness can be asymptomatic, but it often causes gastrointestinal symptoms. Giardia is notable for its resistance to chlorine disinfection, which makes it a concern in many water systems.
Symptoms:
Giardiasis can be asymptomatic but, when symptoms are present, they might include:
- Diarrhea: Especially watery and potentially with a foul odor.
- Fatigue: Feeling tired or weak.
- Stomach cramps and bloating.
- Excessive gas.
- Nausea: Sometimes leading to vomiting.
- Weight loss: Generally due to decreased appetite or malabsorption.
Transmission:
Giardia can be transmitted in several ways, most commonly:
- Contaminated Water: This is one of the most frequent sources of giardiasis, especially in areas where water sanitation practices are not ideal. Drinking or even just swimming in contaminated water can lead to the ingestion of cysts.
- Food: Consuming food that has been in contact with contaminated water or has been handled by someone infected with Giardia can lead to infection.
- Person-to-person: The infection can spread through direct contact with an infected individual. This is especially common in places where hygiene might be compromised, like day care centers.
- Animal-to-person: Some animals, particularly beavers and some domestic pets, can carry Giardia. Coming into direct contact with the feces of an infected animal can lead to transmission.
Prevention:
Preventing giardiasis mostly revolves around hygiene and water safety:
- Avoid drinking untreated water from lakes, rivers, or ponds.
- Use water purification tablets or filters when hiking or camping.
- Practice good hygiene, like washing hands frequently and thoroughly, especially before eating or preparing food.
- Ensure that community swimming pools are well-maintained and properly chlorinated.
Treatment:
If diagnosed with giardiasis, doctors typically prescribe antiparasitic medications. The most common treatments include:
- Metronidazole
- Tinidazole
- Nitazoxanide
Whipworms
Whipworm, scientifically termed Trichuris trichiura, is one of the many intestinal parasites that can afflict humans. The worm, so named due to its whip-like shape, is prevalent in regions with tropical climates, particularly in areas with poor sanitation.
Symptoms:
Many people with whipworm infections may not exhibit any symptoms. However, when symptoms do present, they can include:
- Bloody diarrhea
- Frequent or painful defecation
- Abdominal pain
- Nausea and vomiting
- Headaches
- Unintended weight loss
- Fecal incontinence
In severe cases, whipworm infections can lead to rectal prolapse, where the rectum protrudes from the anus.
Transmission:
Whipworm infections generally arise from the ingestion of whipworm eggs. The main transmission routes are:
- Contaminated Soil: Often, the infection spreads when individuals come into direct contact with soil that’s been contaminated with human feces harboring whipworm eggs. Once in contact, it’s easy to ingest the eggs if hands are not thoroughly washed before eating.
- Contaminated Food or Water: Eating uncooked, unwashed, or poorly washed vegetables and fruits or drinking water that’s been contaminated can also lead to infection.
Prevention:
The following preventive measures can help reduce the risk of whipworm infection:
- Practice good hygiene, including washing hands thoroughly with soap and water, especially before eating and after using the bathroom.
- Use proper sanitation systems to dispose of human feces.
- Ensure that drinking water comes from a safe and treated source.
- Cook and/or wash fruits and vegetables thoroughly before consumption.
Treatment:
When someone is diagnosed with a whipworm infection, they’re typically treated with antiparasitic medications, such as:
- Albendazole: Commonly prescribed for various worm infestations, including whipworm.
- Mebendazole: Also widely used for treating whipworm infections.
- Fenbendazole: Another option in some cases.
It’s vital to follow the recommended dosage and duration when taking these medications to ensure the effective eradication of the worms. If you suspect a whipworm infection, it’s essential to see a healthcare professional to get an accurate diagnosis and appropriate treatment.
Roundworms
Roundworms are parasitic organisms that reside within the body. Infections due to these parasites may result in symptoms like diarrhea and fever. The most common types of roundworms in humans are pinworms and ascariasis. While these infections are often associated with travels to places where sanitation and hygiene are lacking, it’s worth noting that children in the U.S. are also susceptible.
Ascariasis: Causes and Symptoms
Ascariasis, a type of roundworm infection, primarily spreads due to inadequate hygiene practices. The worms often thrive in human excrement. The transmission typically occurs when individuals unknowingly touch contaminated surfaces and then touch their mouths. In some cases, one might observe live worms in their stool. If you exhibit symptoms, they might encompass:
- Coughing.
- Interrupted sleep.
- Feverish feelings.
- General restlessness.
- Intense pain in the abdomen.
- Nausea leading to vomiting.
- Breathlessness or wheezing.
- Signs of malnutrition.
- Delays in growth or development.
Fenbendazole protocol to kill parasites
Fenbendazole is commonly employed as an antiparasitic treatment. The typical dosage recommendation is 1 gram for every 10 lbs of body weight, administered consecutively for three days. This cycle is then repeated biweekly for a period of 2-3 months. Research indicates that dosages up to 2000 mg did not result in any harmful side effects. It’s noteworthy that 1 gram of Fenbendazole paste contains 100 mg of the active ingredient. A regimen that some adopt (which may be geared more towards cancer, but is possibly addressing parasitic infections) is to take 222 mg daily for three days, pause for 4-5 days, and then recommence the cycle. In practical terms, try doses of 750 mg or 375 mg, especially when tablets available are 1.5 grams each. If employing horse paste as a source, dosing for a 150-pound individual will equate to approximately 357 mg.
Nitazoxanide, commercially known as Alinia, can be bought from international pharmacies. The suggested dosage is 500 mg, twice daily for adults, taken over a three-day span. This regimen should be repeated every 5-7 days for a duration of 1-2 months or more if necessary. It’s believed to be effective against various parasite forms and also has antiviral properties.
How does fenbendazole work for parasites?
Fenbendazole functions as an antiparasitic agent by targeting the parasite’s cellular structure. Specifically, it binds to the beta-tubulin proteins within the microtubules of the parasite. Microtubules play an essential role in cell division and maintaining cell shape. When Fenbendazole binds to these proteins, it hinders the formation of these microtubules. This interference with microtubule assembly disrupts the parasite’s cell division process. As a result of this disruption, the parasite’s energy production mechanism is compromised. Deprived of its primary energy source, the parasite ultimately starves and dies, thus effectively eradicating the infection.
Diet and Supplements for Parasite Prevention
Dietary Choices:
- Minimize intake of simple carbohydrates, found in refined foods, fruits, dairy products, juices, and sugars, excluding honey.
- Incorporate foods known for their anti-parasitic properties such as raw garlic, pumpkin seeds, pomegranates, beets, and carrots. A combination of honey and papaya seeds, for instance, has been shown to eliminate parasites in a majority of study participants.
- Stay hydrated. Drinking ample water aids in flushing out toxins and parasites from the body.
- Boost your fiber intake. Dietary fiber can assist in expelling worms from the digestive tract.
Supplements:
- Probiotics: Including Lactobacillus acidophilus, Lactobacillus plantarum, Saccharomyces boulardii, and bifidobacteria. These friendly bacteria fortify the digestive system. However, they may not be suitable for everyone, especially those with severely compromised immune systems. It’s best to consult a healthcare provider.
- Digestive Enzymes: These can restore the balance in your gut, making it unfavorable for parasites. Papain, an enzyme derived from the papaya fruit, can potentially aid in eradicating worms when consumed around meal times. Caution is needed for individuals with bleeding disorders or those on anticoagulant medications, like warfarin.
- Vitamin C: An immune booster. However, excessive intake might result in diarrhea, so adjust the dose accordingly.
- Zinc: Another immune system ally. Be aware that zinc can interfere with certain medications, notably some antibiotics, and may not be suited for those with conditions like HIV/AIDS. Always consult with your physician before making changes to your supplement regimen.
FREQUENTLY ASKED QUESTIONS
How do adults get worms?
Adults can become infected with worms in various ways. Consumption of raw or undercooked meat and seafood is a common source. Swimming in or ingesting contaminated water can also introduce these parasites. Additionally, walking barefoot in areas where worms thrive can lead to infections. Everyday activities, such as sharing items like clothing or bedding, can be risky, especially if proper hygiene practices, like regular handwashing, aren’t followed.
What do intestinal worms feed on?
Intestinal worms primarily consume nutrients present within the intestines. As they absorb these nutrients, they can deprive the host, leading to malnutrition or other nutrient-related issues.
What does feces look like when you have worms?
If someone has worms, their feces might sometimes show signs of the infection. Some individuals might notice diarrhea or constipation. In certain instances, one might even spot a whole worm or fragments of it in the fecal matter. However, many times, the infection can be asymptomatic, showing no clear signs.
Does fenbendazole kill parasites in humans?
Fenbendazole, known chemically as [5-(phenylthio)-1H-benzimidazol-2-yl] carbamic acid methyl ester, is a widely recognized treatment for various parasitic infections. This includes pinworms, helminths, and other parasites found in laboratory animals, livestock, pets, and indeed, humans.
Does fenbendazole kill all parasites?
Fenbendazole is effective against a variety of parasites, but it doesn’t target all. For instance, it isn’t the recommended treatment for tapeworms that fleas transmit. If a person or animal still exhibits signs of a parasitic infection after fenbendazole treatment, a different deworming medication might be needed.
What happens when a parasite dies in your body?
When parasites die, they can release toxins, which might result in unpleasant symptoms. This can feel overwhelming for the body, especially if many parasites die simultaneously. Symptoms, which can seem like a worsening condition, are actually indicators of the body’s healing process. It’s termed as “die-off” symptoms. To manage these, consider regular massages, adequate hydration, and ensuring quality sleep. Consultation with a healthcare professional is vital. They can provide guidance on whether activated charcoal, bentonite clay, or even enemas might help alleviate these die-off symptoms.














How does this work on stage 4 Cancer
Fenbendazole stopped my metastasis. Tumors have not grown. Lungs are working at 100%. Stage 4. Breast lung and lymph nodes. 2 years. All natural. Never used chemo radiation or immunotherapy. Coffee enemas rejuvenate the liver by cleaning out the bile ducts. Liver is the most important organ.
After using fenbendazole i saw some parasites that were large enough to see in my toilet. Also a stool sample found different species of parasites that were only visible under a microscope. You cannot see all parasites with your eyes!
Has anyone seen parasites or worms in your stool while taking fenbendazol
Yes! Mine looks like little rocks the size of sunflower seeds
Yes, I saw two types – one was a rice grain looking thing. The other looked like a small piece of broken thin spaghetti.
I’ve read a few articles saying that doctors have “discovered“ that nearly every person with cancer has parasites, so of course a parasite cleanse only makes sense at least from time to time.
Do parasites present as cysts sometimes? Husband has been on the protocol for a month and last night a cyst he has had since a teen just ruptured.
Can you take fenbendazole just as a parasite cleanse medication? Not have cancer but hate to think I have parasites. I don’t have a gall bladder, but I have gastrointestinal diseases.